Magnetic resonance imaging is a diagnostic method that provides a detailed picture of the nature of pathological changes in any area of the human body.
In orthopedic practice, the most common MRI of the hip joint is performed to clarify the causes of coxalgia – pain syndrome in the joint. The research method does not use ionizing radiation, which is particularly relevant for children and pregnant women. The process of creating clear images that can be enlarged and viewed in volumetric view is based on magnetic resonance and computer technologies. Contrast enhancement is used to improve imaging skills. The diagnostic value of the photos obtained after the gadolinium injection is comparable to the results of arthroscopy – an invasive study of penetration into the joint cavity with surgical instruments.
How is hip joint MRI done? Scans are carried out on machines with different magnetic field strengths. The doctor can select the programs regardless of the clinical goals. This is relevant if at first it is not clear what is causing the pain syndrome: pelvic organ pathology or joint pathology. Multiparametric sequences are used in standard situations.
Hip joint diseases on MRI
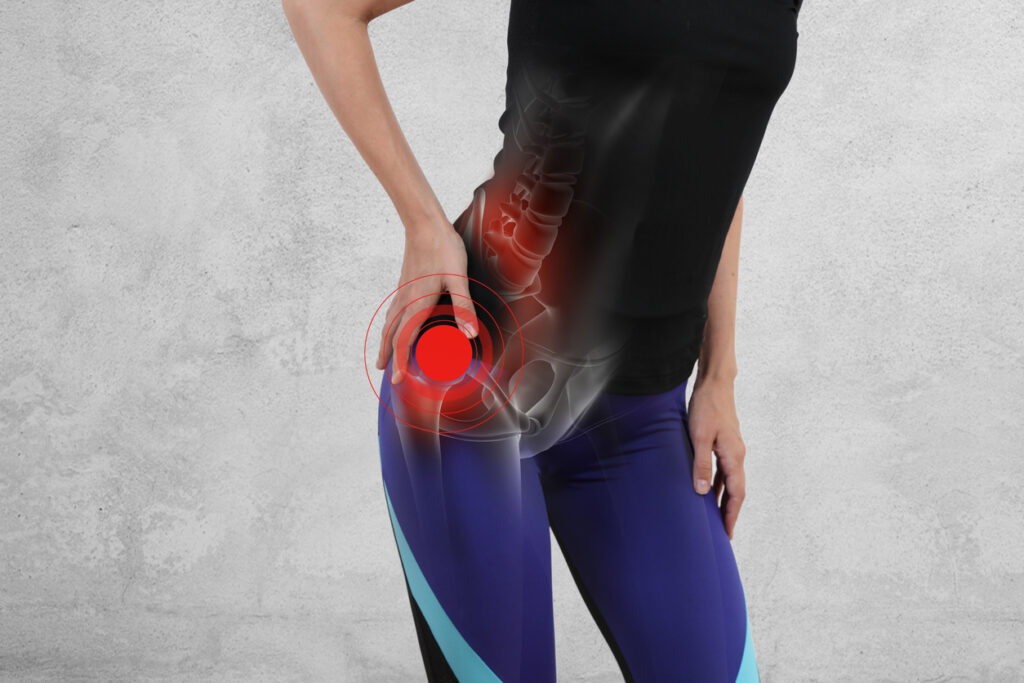
Source: vanthielmd.com
Magnetic resonance scans are used to diagnose a number of pathological conditions. What does an MRI scan of the hip joint show? Visualize the scans
- Femoroacetabular Impingement Syndrome.
A mechanical conflict between the femoral head / neck and socket rim is caused by unilateral or bilateral bone defects of congenital or acquired origin. Modified components of the articulation cause extremity dysfunction by collision during movement. Pathological friction of the bones contributes to the growth of osteophytes against the background of constant traumatization of the acetabulum. If the disease is not diagnosed in time and treatment is not started, it will eventually tear and the cartilage tissue of the joint bones will be destroyed. Such a mechanical conflict often contributes to the formation of coxarthrosis and is accompanied by progressive pain syndrome.
The MRI of the hip joint in femoroacetabular impingement syndrome shows the possible causes of the disease:
- congenital malformations;
- Complications after trauma and surgery;
- accompanying avascular necrosis of the femoral head;
- inflammatory processes in the synovial sac;
- Osteochondropathy (Perters disease);
- Epiphysiolysis (Salter-Harris fracture);
- Atrophied muscles around the joint, etc.
In a severe form of diabetes mellitus with circulatory disorders, regular physical overload, concomitant diseases of the musculoskeletal system and connective tissue (arthritis, gout, systemic lupus erythematosus, etc.), bone and cartilage structures are destroyed.
Arthrosis. A pathological process over many years leads to the complete loss of function of the hip joint due to the destruction of all joint components. Changes in bone tissue, ligaments, blood vessels, cartilage, and surrounding muscles can be seen on an MRI with contrast agent. Involvement of nerve bundles causes persistent hip pain. Predisposing factors are:
- endocrine disorders;
- Practicing heavy sports;
- Obesity;
- Associated arthritis, osteoarthritis, etc.
The disease has three degrees of severity. Hip MRI shows changes at an early stage when it is possible to prevent / slow the progression of the pathology with the help of drug therapy.
- Avascular necrosis of the femoral head.
The development of avascular necrosis is caused by a prolonged interruption in nutrition of the hip joint against the background of blood thickening, thrombosis, compression and twisting of the vessels. The ischemia creates cavities in the bone tissue that lead to deformations and detachment of cartilage. Clinical manifestations are unspecific and cause difficulty in diagnosis. There are many provoking factors:
Early changes are not visible on X-rays or ultrasound. Hip MRI is one of the most effective ways to detect the disease in its early stages.
Both benign and malignant tumors can develop in the hip joint. The MRI photo shows the presumed nature of the tumor. Reviewing the diagnosis requires a biopsy. Pain occurs when nerve endings, border tissues, and vessels are compressed, which is the case with any tumor, so the absence of symptoms should not delay the MRI. Primary bone neoplasms can be better diagnosed by CT scans, MRI is better suited for detecting changes in the soft tissue.
Hip MRI: indications and contraindications
Source: medicalnewstoday.com
Endoprostheses can cause image errors, so roentgen diagnostic methods are preferred.
MR tomography is carried out in the event of ambiguous results from computer scanning, radiography, ultrasound. The method is suitable for dynamic observation: In the case of medical indications, there are no restrictions on the number of MRI images. The clinical manifestations of a number of pathological processes are similar, and advanced diagnostics are needed to determine the exact genesis of symptoms. Indications for hip MRI are:
- Persistent pain syndrome, inexplicable claudication, discomfort when walking and / or at rest, restricted movement in the joint;
- No effect / short-term improvement against the background of the therapy;
- Assessment of post-traumatic complications – in an emergency, the search begins with a CT scan;
- primary detection of diseases – inflammation, destruction, tumor pathology, congenital abnormalities, infectious lesions, degenerative-dystrophic processes, etc .;
- Examinations before and after surgery – endoprosthetics, etc .;
In the case of pain related to neuralgia, the MRI of the hip joints shows normal, the study is carried out to differentiate the processes.
Contraindications for the MRI examination:
- Presence of implanted devices in the body – myo-, neuro-, cardiac pacemaker, defibrillator, insulin pump, permanent hearing prosthesis, metal vascular clips with paramagnetic properties, Ilizarov apparatus, etc .;
- Pregnancy in the first trimester;
- Children under one month;
- Obesity with body weight over 120 kg (for scanners with closed contour);
- severe well-being of the patient due to an acute condition: pain syndrome on the background of trauma, heart attack, stroke, etc .;
- Inability to remain in the supine position for a long time;
- some psychological and neurological pathologies – alcohol delirium, epilepsy, claustrophobia, Parkinson’s disease, Alzheimer’s (MRI is performed in hospital conditions under sedation).
No contrast agent study is available for patients with a history of allergic reactions to gadolinium, end-stage renal disease, and pregnant women of any age. Permanent tooth structures – veneers, pins, braces, titanium endoprostheses do not prevent the MRI examination
How do I get an MRI of a hip joint?
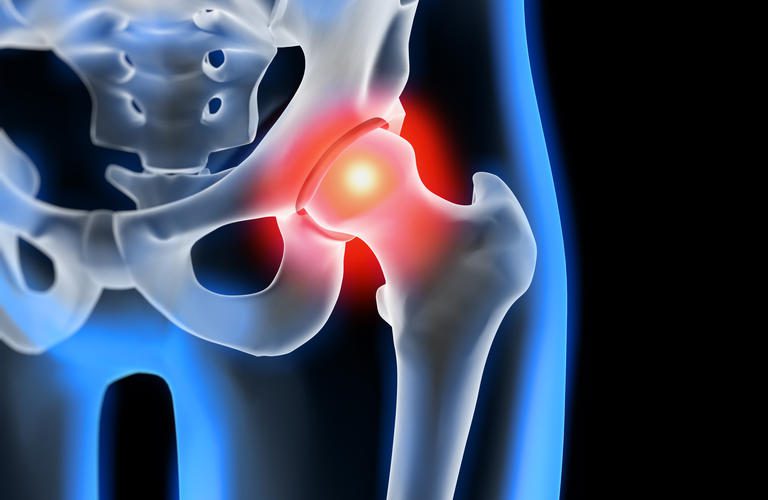
Source: hueftspezialist.de
To improve the signal-to-noise ratio, the problem area should be as close to the center of the table as possible
Magnetic resonance imaging of the mentioned joint is carried out on various devices. Images obtained on the device with a closed contour are more informative. The best option is an MRI examination on a closed scanner with a magnetic field strength of 1.5 Tesla or more. Low-power devices are used for screening diagnostics of athletes when there are no symptoms. More information on the site https://mricfl.com.
The patient comes to the clinic 20 minutes before the examination. After the paperwork has been done and objects containing metal have been put down, the X-ray technician places the patient on the CT scanner table.
During diagnosis, one or two hip joints can be considered, depending on the indication: Systemic diseases imply a complex examination of several areas.
The patient is placed on their back with their big toes brought together to allow rotation of the hip joints. A hamstring roll and a soft fixation of the extremities with straps are used to prevent accidental movements. A coil is placed over the area of interest. When contrast agent is planned, a catheter is inserted into the ulnar vein and an automatic injector is connected: at a preset time, the enhancer agent is delivered into the body.
After evaluating the targeted images, the radiologist selects the right one MRI sequences. The diagnostic process is monitored by medical staff through a window in a nearby room, communication takes place via a hands-free device. If the patient’s condition worsens, the scan can be paused; the patient has a special button at hand. When the scan is complete, the patient is usually given a conclusion and a diskette with a record of the diagnostic procedure. The video can be opened with a program that supports the Dicom format.
How do you prepare for a hip MRI?
Source: medicover.hu
No special measures are required, it is enough to put down metal objects (keys, coins, etc.), payment cards, jewelry, watches, wear loose clothing without zippers and rivets. Bring a package with documents: passport, descriptions of the results of the previous diagnostics, medical referral, health insurance policy (if payment is made through an insurance company).
Injection of contrast agent into the body very rarely causes clinically significant side effects, but in 8-10% of cases vegetative reactions – salivation, Dizziness, nausea, etc. – are recorded. To prevent such phenomena, it is necessary to have a snack 15 minutes before leaving the house.
For women who are breastfeeding, preparing for the MRI of the hip with contrast agent means a reserve of milk for several feedings. An intensified drinking cure after the diagnostic procedure helps to get rid of gadolinium chelates faster.
How is a hip MRI done when internal organs also need to be viewed? If there is a suspicion of a possible pathology of the uterus, limbs, prostate, seminal vesicles, or supportive pain syndrome, the preparation of the study includes cleaning the intestines and eliminating gas. The bladder is scored when it is full.
Thank You For Reading!
Reference: soundhealthdoctor.com
