
By Lauren Weber, Kaiser Health News
Rural Americans are more than twice as likely to die from Covid as their urban counterparts – a gap health experts say is likely to widen as access to health care shrinks for a population that tends to be older, sicker, heavier, poorer and less vaccinated .
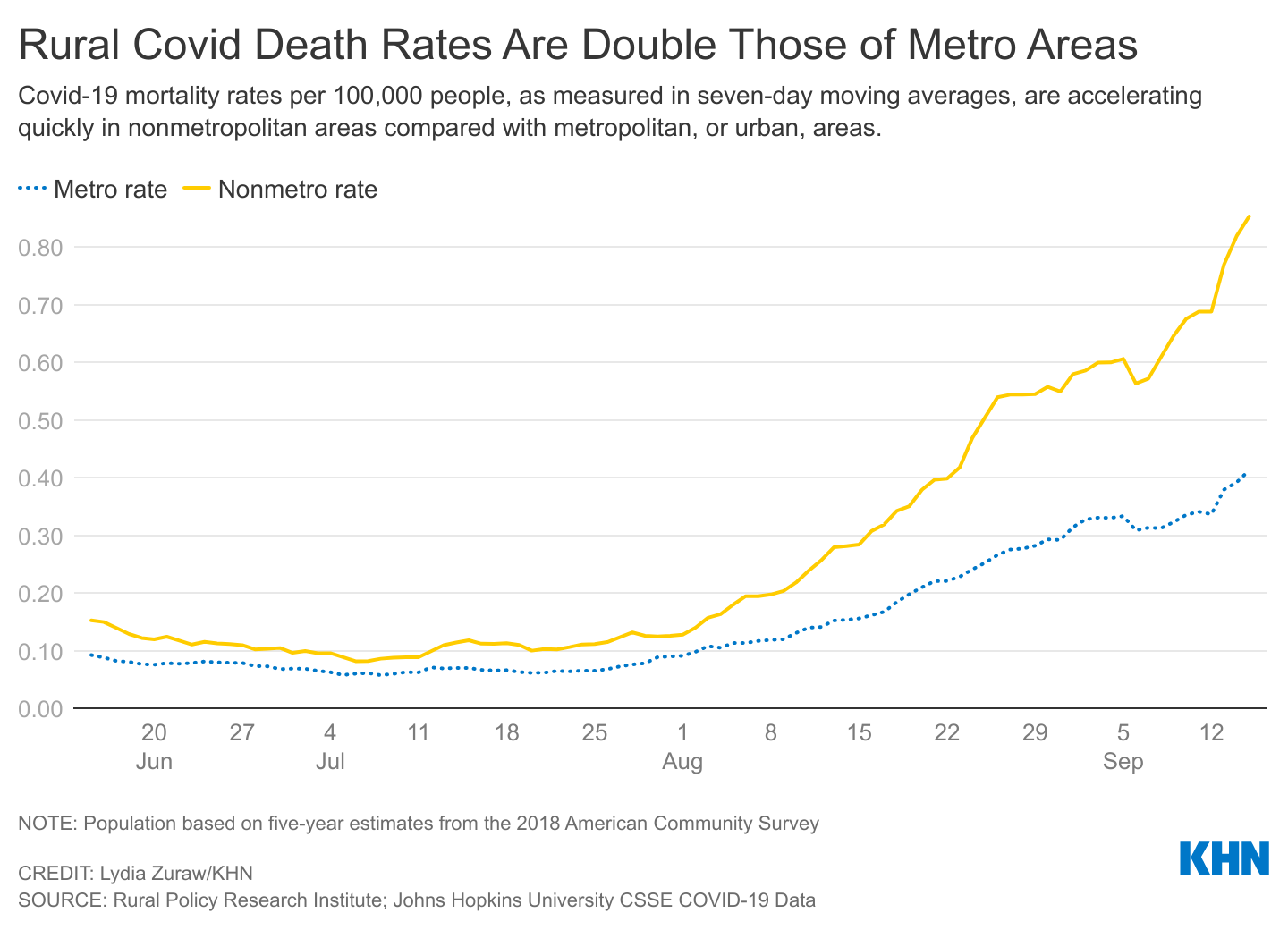
During the initial surge in Covid-19 deaths skipped much of rural America where approx. 15% of Americans are alive, death rates outside of metropolitan areas quickly exceeded those in metropolitan areas as the virus spread nationwide before vaccinations became available, according to data from the Rural Policy Research Institute.
Since the pandemic began, about 1 in 434 rural Americans have died of Covid, compared with about 1 in 513 urban Americans, the institute’s data shows. And although vaccines have lowered overall death rates from Covid infections since the winter high, mortality rates in rural areas are now more than double those in cities – and are accelerating rapidly.
In rural northeast Texas, CEO of the Titus Regional Medical Center Terry Scoggin fights in his community with a vaccination rate of 39%. Eleven patients died of Covid in the first half of September in his Mount Pleasant hospital, which has a population of 16,000. Typically three or four non-hospice patients die there in a whole month.
“That’s not how we see death,” said Scoggin. “You don’t usually see your friends and neighbors die.”
Part of the problem is that September Covid incidence rates in rural areas were about 54% higher than elsewhere, said Fred Ullrich, a research analyst from the University of Iowa’s College of Public Health who co-authored the institute’s report. He said the analysis compared the rates of non-metropolitan areas, or rural, Areas and metropolitan or urban areas. In 39 states, he added, rural counties had higher rates of Covid than their urban counterparts.
“There is a national gap between perception and reality when it comes to Covid in rural America,” said Alan Morgan, Head of the National Rural Health Association. “We have turned many rural communities into killer boxes. And there is no movement towards what we see in many of these communities, either in public or among government officials. ”
However, the high incidence of cases and low vaccination rates do not fully capture why mortality rates are so much higher in rural areas than elsewhere. Academics and officials alike describe the higher rate of poor health among rural Americans and their limited health care options as a deadly combination. The pressures of the pandemic have exacerbated the problem by exacerbating staff shortages in hospitals, creating a cycle of deterioration in access to care.
It’s the latest example of the deadly coronavirus causing more damage in some communities than others. Covid has also killed Native Americans, blacks, and Hispanic Americans disproportionately high rates.
Vaccinations are the most effective way to prevent Covid infections from being fatal. About 41% of rural America was vaccinated as of September 23, compared to about 53% of urban America Analysis by The Daily Yonder, a newsroom for rural America. Limited supplies and poor access made it difficult to get gunshots in the far-flung regions at first, but officials and academics are now blaming vaccination reluctance, misinformation and politics for low vaccination rates.
In the hard-hit southwest of Missouri, for example 26% of Newton County’s residents were fully vaccinated on Sept. 27. The Department of Health held raffles and vaccination clinics, announced it in the local newspaper, and even brought the vaccine to those who do not have transportation in remote areas, according to department head Larry Bergner. But he said interest in the recordings usually only rises when someone in the social circle of a reluctant person dies or becomes seriously ill.
In addition, the congestion of Covid patients in hospitals has undermined a fundamental tenet of rural health infrastructure: the ability to move patients from rural hospitals to higher levels of specialized care in regional or urban health centers.
“We literally have email listservs from rural chief nurses officers or rural CEOs sending an SOS to the group and saying, ‘We’ve called 60 or 70 hospitals and we can’t get this heart attack or stroke patient or surgical patient out and them “’Will become septic and die if it lasts much longer,'” said John Henderson, President and CEO of Texas Organization of Rural and Community Hospitals.
Morgan said he couldn’t count how many people talked to him about the transfer problem.
“It’s crazy, just crazy. It’s unacceptable, “said Morgan.” From what I see this mortality gap is accelerating. ”
Access to health care has long ravaged parts of rural America – since 2005 181 rural hospitals have closed. A 2020 KHN analysis found that more than half of the US counties, many of them, mostly rural, do not have a hospital with intensive care beds.
According to 2019 data from the Centers for Disease, rural Americans had 20% higher overall mortality rates than those living in urban areas before the pandemic due to their lower insurance rates, higher poverty rates, and more limited access to health care control and prevention National Center for Health Statistics.
In Ripley County, southeast Missouri, the local hospital closed in 2018. From September 27th only 24% of the residents were fully vaccinated against Covid. Due to the recent number of cases, Covid patients are being sent home from emergency rooms in the surrounding counties if they are not “badly ill,” said Health Department Director Tammy Cosgrove.
The shortage of care that hits the country is particularly severe in rural areas, which have less money than large hospitals to pay the exorbitant fees that travel nursing agencies charge. And with nursing temporary employment agencies offering hospital workers more money to join their teams, many rural nurses are dropping out. One of Scoggin’s nurses told him she had to get a traveling job – with that much money she could pay off her debt in three months.
And then there is the burnout if you work for over a year and a half during the pandemic. Audrey Snyder, the immediate former president from the Rural Nurse Organization said she stopped counting how many nurses told her they were quitting. These layoffs create an inexorable cycle: As travel nurses attract more and more nurses, the nurses who have to shoulder their jobs get burned out – and eventually quit. While this applies to hospitals of all types, the effects can be particularly severe in hard-to-fill rural hospitals.
Rural health authorities are scared the lack of staff could be made worse by health care Vaccination mandates promised by President Joe Bidenthat they say are a. could cause Wave of resignation the hospitals cannot afford it. About half of Scoggin’s employees, for example, are unvaccinated.
Snyder warned that the shortage of nursing staff and the associated high costs will no longer be sustainable for rural hospitals, which operate on wafer-thin margins. She predicted that a new wave of hospital closures in rural areas will continue to drive dire mortality rates up.
The staff shortage already limits the number of beds hospitals can use, Scoggin said. He estimated that most Texas hospitals, including his own, operate on about two-thirds of their bed capacity. His emergency room is so crowded that he had to send a few patients home every day to be monitored by an ambulance.
KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism on health topics. Along with Policy Analysis and Polling, KHN is one of the three main operational programs at KFF (Kaiser Family Foundation). KFF is a non-profit foundation that provides the country with information on health issues.
Subscribe to to the free morning briefing from KHN.
.
Thank You For Reading!
Reference: www.healthywomen.org
